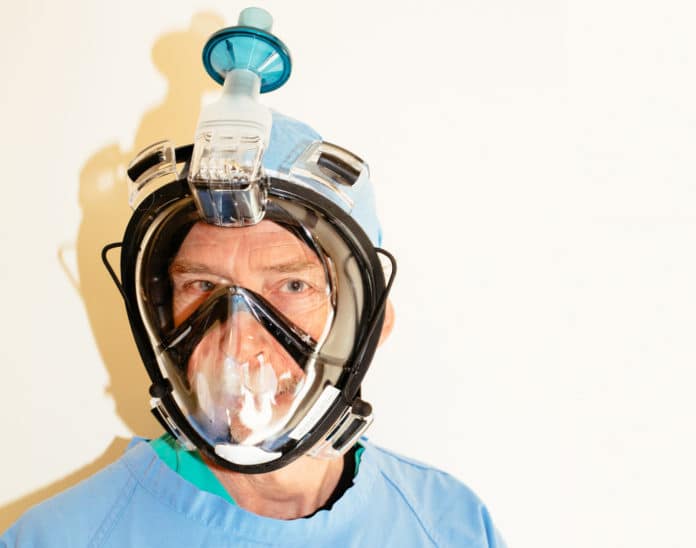
One of the things we are seeing a lot of is people our age innovating small, incremental improvements that, when taken together, are having a big impact. These are not the sort of innovations that show up on graphs of infection projection. But they are the sort of small improvements that are incredibly meaningful in the long run. The pandemic is shockingly bad in its impact on everyone, but people like Dr. Ruth Zimmer 58, and her group, give us a sense of optimism for what can happen when smart people around the world are creating novel solutions to help us all.
Innovative Physician Anesthesiologist Moms
Dr Zimmer, when did you first learn about these masks?
I belong to a Facebook group called PAMG (physician anesthesiologists mom group). We share information and commiserate on everything from breastfeeding to dealing with the emotional consequences of a patient’s death or a surgeon’s obtuseness. In late February/ early March members of this group began dealing with COVID-19 patients in Washington State. They quickly ran out of PPE and needed to improvise in order to protect themselves from potential infection. The government and administrators were slow to adjust and so the efforts fell to the individuals.
We have members of this group from all over the world and I began seeing that in Italy (I think) some people were DIYing things that have traditionally been used for other purposes. It was on one of those posts that I first saw the remarkable concept of using a snorkeling face mask with modifications to attach a viral filter.
What is their original usage?
I had not seen these before, because I don’t spend a lot of time in or near the ocean, but these masks are widely used for snorkeling. They are really quite ingenious. You can snorkel with full face coverage and not worry about fogging of the mask. You don’t have to have a snorkel with a mouthpiece and I am definitely getting some of these for snorkeling when this pandemic subsides.

One Snorkel Replaces Three Pieces of PPE
What is the advantage of them vs more conventional PPE?
We have found that they protect your face better than using multiple pieces of PPE. One piece of protective equipment replaces three. The mask with a filter replaces the N95, a face shield or another mask to cover the N95 (for extending use), and goggles.
In practice, it is more comfortable for extended use, covers and seals the face (so no touching the face), it makes the work of breathing easier than an N95, and people seem to retain less CO2 resulting in less headaches and fatigue.
How do people re-use them?
The recommendation is to use one all day during aerosol-generating procedures. So if you are in a cohorted ICU you can wear it all day while taking care of COVID-19 patients. If you are in an operating room you can wear it during the whole case or you can wear it only for the risky parts of incubation and extubation (aerosol-generating procedures). The filter can be used for days but should be changed between individuals who are using the mask. The mask itself can be wiped down with ETOH or bleach cloth or washed in soapy water.
How many of them did you get?
I was given 200 to share with my colleagues.
Creative and Thoughtful Research
Who gave them to you? and why?
Mark Siu with Wildhorn gave them to me. Like many people who feel so at a loss for how to help with this pandemic, he wanted to do what he could to help. He had been selling them online and realized that he was quickly running out of product. He reserved a few hundred to help out the front-line care givers in his community. I was connected with Mark through a friend who used to be a resident under me when I was attending at the University of Utah. This friend (Sean Runnels) had a colleague at the university who was working with a research group out of Stanford, headed by Manu Prakash, that is trying to prove the safety and effectiveness of the product. I have since joined this open-source study group as a clinician. They are doing research on the fly; it is thoughtful and effective and relevant research. I had become somewhat jaded with research, it seemed so esoteric and not applicable, but this group has renewed my faith in the concept of research being a creative, thoughtful, and scientific exploration of what is possible.
I don’t know if anyone has been infected while wearing one of these, but if you think through their function you can draw some conclusions. The face-shield component is sealed plexiglass. The sealed plexiglass is a better barrier than an open shield. The viral filter is the same one we use to keep our anesthesia machines clean and it filters 99.9% of bacteria and viruses. The N95s have to be fit tested. This is a qualitative test that can easily be performed on the mask as well. N95s become moistened when used for prolonged periods of time and then are ineffective; they can become misshaped with face movement and the seal is really only over the nose and mouth.
Extensive Clinical Testing
Are they being tested and how?
Stanford, the University of Utah, and a few others around the country are doing extensive laboratory and clinical tests to ensure safety and function. Some of the tests involve exercising with the masks on to evaluate for air flow and work of breathing. Other tests are being performed that are quantitative evaluations of the seal in preventing entrainment of room air. The N95s that we wear are only qualitative tests and not quantitative so this is a step beyond what we get with N95s.
The masks are sturdy and built for reuse. PAPRs (Powered Air Purifying Respirator), which are the closest in coverage to the masks, seem to be more vulnerable to individual care.

Do you know if it is possible to get thousands of them?
There are tens of thousands of these being shipped around the country and world right now.
How are you and your team handling the pandemic so far in Utah?
We are in a preparing-and-waiting mode right now. As a state, we began addressing social distancing early and took it seriously. Intermountain Healthcare and my group Mountain West Anesthesia also began preparing for worst case scenarios early. Because of all the precautions and preparation, we are prepared and I believe will weather this storm better than many. As Mike Leavitt (director of HHS 05-09) has said, “Everything we do before a pandemic will seem alarmist. Everything we do after will seem inadequate.” Mike Leavitt was also the governor of Utah from 1992-2003. He is very respected in Utah and his words carry weight so the state was prepared to follow his lead.
My group and Intermountain are in a position of watchful waiting. The surge has not yet arrived and we are not sure what it will be when it does, but we have enough people sitting and waiting that some are heading to NYC to help out there.